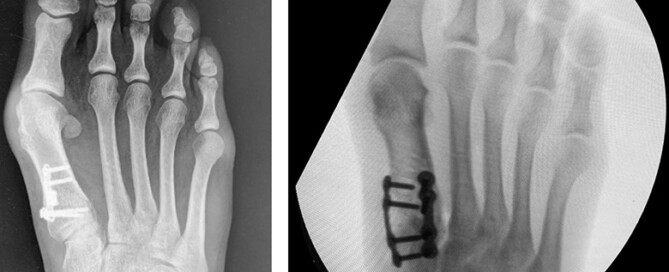
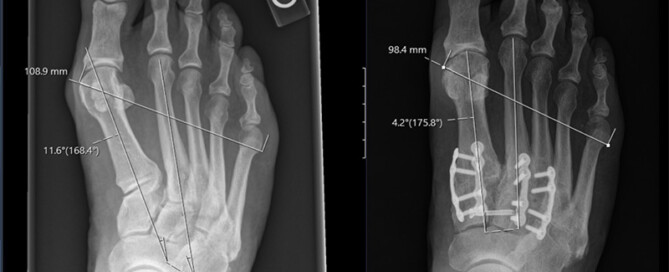
Has Bunion Surgery Failed You? Here Is Your Ultimate Guide to Fixing Bunions Again, The Right Way This Time!
Hey, Let's Talk Bunions... Again So, you had bunion surgery and thought you were done with the whole ordeal, but your bunion decided to make a comeback. Well, don't lose hope. I'm here to talk about an exciting and effective method called Lapiplasty. This could be the solution you've been looking for! First Off, What [...]